Senior Nutrition & Meal Planning: A Home Care Agency Guide
A comprehensive senior nutrition guide covering daily nutritional needs, common deficiencies, hydration, modified diets, meal planning for seniors, and community resources. Built for home care agencies and caregivers supporting nutrition for elderly at home. Meal preparation is one of the key instrumental activities of daily living (IADLs) tracked in home care assessments. Nutritional observations should also be documented in each patient's care plan.

Nutritional Needs of Older Adults
As people age, their nutritional needs change. Elderly nutrition requires more attention to protein intake, micronutrient density, and hydration, often while consuming fewer total calories. Understanding these changes is essential for effective meal planning for seniors.
Caloric Needs Decrease
Metabolic rate drops 1-2% per decade after 20. Seniors need fewer calories but the same or more nutrients, making nutrient-dense food choices critical.
Protein Needs Increase
Older adults need 1.0-1.2 g/kg/day of protein (vs 0.8 g/kg for younger adults) to maintain muscle mass and prevent sarcopenia. Even higher for illness or wounds.
Hydration Is Critical
Thirst perception decreases with age. Dehydration is a leading cause of hospitalization in seniors and can cause confusion, UTIs, and falls.
Nutrient Absorption Declines
Stomach acid and intrinsic factor decrease, reducing absorption of B12, calcium, iron, and zinc. Medications can further impair nutrient uptake.
Fiber Remains Essential
Most seniors consume only half the recommended fiber. Adequate fiber prevents constipation, supports heart health, and helps manage blood sugar.
Vitamin D Is Often Deficient
Reduced sun exposure, skin synthesis, and dietary intake make vitamin D deficiency the most common nutritional issue in older adults (up to 42%).
Daily Nutrition Calculator for Seniors
Enter patient information below to get estimated daily nutritional needs. This senior nutrition guide tool provides general estimates based on age, sex, weight, and activity level.
Estimated Daily Needs
1336
kcal/day
Calories
82
g/day
Protein
69
oz/day
Fluids
21
g/day
Fiber
These are general estimates based on the Mifflin-St Jeor equation and USDA guidelines. Actual needs vary by health conditions, medications, and individual metabolism. Always consult with a registered dietitian for personalized elderly nutrition plans.
Common Nutritional Deficiencies in Seniors
Nutritional deficiencies are widespread among older adults and can significantly impact health outcomes. Identifying and addressing these gaps is a key part of any senior nutrition guide for home care agencies.
Vitamin D
42% of seniors affectedImpact: Bone loss, increased fall risk, weakened immunity, depression
Sources: Sunlight, fortified milk, fatty fish, eggs, supplements
Vitamin B12
10-30% of seniors affectedImpact: Anemia, fatigue, cognitive decline, neuropathy, confusion
Sources: Meat, fish, dairy, fortified cereals, supplements
Calcium
25-30% of seniors affectedImpact: Osteoporosis, fractures, muscle cramps, dental problems
Sources: Dairy, fortified plant milks, leafy greens, sardines
Fiber
50%+ of seniors affectedImpact: Constipation, increased cholesterol, blood sugar instability
Sources: Whole grains, fruits, vegetables, legumes, nuts
Protein
30-40% of seniors affectedImpact: Sarcopenia (muscle loss), slow wound healing, weakened immunity
Sources: Meat, poultry, fish, eggs, dairy, beans, soy
Potassium
35%+ of seniors affectedImpact: High blood pressure, irregular heartbeat, muscle weakness
Sources: Bananas, potatoes, beans, spinach, yogurt
Hydration: A Critical Part of Elderly Nutrition
Dehydration is one of the most common and preventable problems in senior care. Older adults lose their sense of thirst, making intentional hydration tracking essential for caregivers managing nutrition for elderly at home.
Daily Hydration Tracker
Track daily fluid intake. Each glass represents approximately 8 oz (240 mL). Target: 8 glasses per day.
Signs of Dehydration in Seniors
- Dark-colored urine or decreased urination
- Dry mouth, lips, and tongue
- Confusion or increased agitation
- Dizziness or lightheadedness
- Constipation
- Sunken eyes
- Rapid heart rate
- Poor skin turgor (skin tenting)
Hydration Strategies for Caregivers
- Offer fluids at every interaction and between meals
- Keep water visible and within reach at all times
- Serve water-rich foods: watermelon, cucumber, soup, gelatin
- Flavor water with fruit slices if plain water is refused
- Use cups and straws that are easy to hold and sip from
- Track intake with a simple log (like the tracker above)
- Set reminder alarms for fluid offerings every 1-2 hours
- Address fear of incontinence with bathroom schedule
Diet Modification Reference Cards
Many seniors require modified diets based on their medical conditions. These interactive reference cards provide quick guidance on common therapeutic diets used in meal planning for seniors.
Meal Preparation Tips for Caregivers
Effective meal planning for seniors requires attention to safety, nutrition, and the patient's preferences and abilities. These strategies help caregivers provide nutritious meals efficiently.
Cooking & Preparation
- Batch cook and freeze meals in individual portions for the week
- Use slow cookers and instant pots for tender, easy-to-chew meats
- Pre-cut fruits and vegetables for easy snacking
- Label all containers with contents and date prepared
- Use color-coded cutting boards for food safety
- Keep commonly used items at waist height for accessibility
Food Safety
- Refrigerate leftovers within 2 hours of cooking
- Use a food thermometer: poultry 165 F, ground meat 160 F, leftovers 165 F
- Discard food left at room temperature for more than 2 hours
- Wash hands for 20 seconds before and after handling food
- Check expiration dates regularly; seniors may not notice spoiled food
- Clean refrigerator weekly; keep at 40 F or below
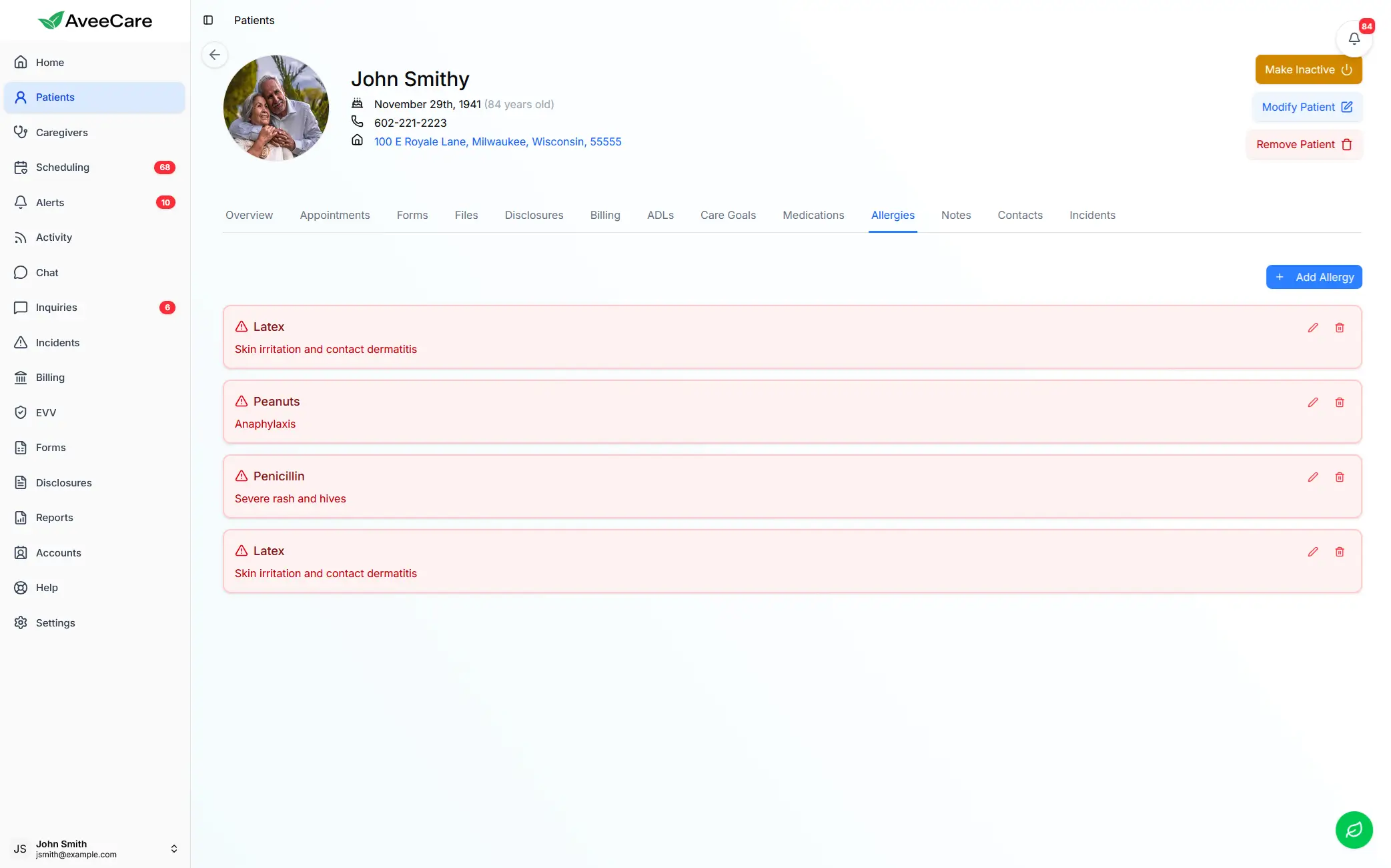
AveeCare's allergy and dietary tracking helps agencies manage elderly nutrition and diet restrictions
Appetite Stimulation Strategies
Loss of appetite is one of the most common challenges in elderly nutrition. Multiple factors contribute, including medications, depression, dental issues, and decreased taste and smell. These evidence-based strategies can help.
Serve Smaller, Frequent Meals
Offer 5-6 small meals per day instead of 3 large ones. Large portions can feel overwhelming. Keep nutrient-dense snacks accessible between meals.
Enhance Flavor Naturally
Use herbs, spices, lemon juice, and vinegar to boost flavor. Taste perception decreases with age, and many medications alter taste. Avoid relying on salt.
Make Meals Social
Eating alone is strongly associated with reduced intake. Encourage shared meals with family, friends, or other seniors. Congregate dining programs can help.
Boost Calorie Density
Add olive oil, butter, nut butters, cream, or cheese to meals. Powdered milk can be added to soups and smoothies for extra protein and calories without extra volume.
Address Dental Issues
Ensure dentures fit properly. Oral pain or poorly fitting dentures are a leading cause of poor nutrition in seniors. Schedule regular dental checkups.
Time Meals Strategically
Serve the largest meal when the patient has the most energy (often breakfast or lunch). Offer a lighter dinner. Avoid heavy meals close to bedtime.
Community Nutrition Resources for Seniors
Multiple federal and community programs exist to support nutrition for elderly at home. Home care agencies should be familiar with these resources to connect clients with supplemental nutrition assistance.
Meals on Wheels
Home-delivered meals for homebound seniors 60+. Also provides wellness checks and social interaction. Over 5,000 local programs nationwide serve 2.4 million seniors annually.
mealsonwheelsamerica.org
SNAP (Food Stamps)
Supplemental Nutrition Assistance Program. Seniors 60+ may qualify based on income. Average benefit is $104/month per person. Application through local SNAP office or online.
fns.usda.gov/snap
Congregate Meal Programs
Free or low-cost group meals at senior centers, churches, and community centers. Provides socialization alongside nutrition. Funded under the Older Americans Act.
Local Area Agency on Aging
Senior Farmers' Market Nutrition Program
Provides low-income seniors with coupons for fresh fruits, vegetables, herbs, and honey at farmers' markets. Available in most states during growing season.
fns.usda.gov/sfmnp
Frequently Asked Questions
Common questions about elderly nutrition, meal planning for seniors, and nutrition for elderly at home.
Sources & References
This senior nutrition guide draws on federal dietary guidelines and authoritative nutrition resources.
Federal dietary guidance including specific recommendations for older adults.
Evidence-based information on vitamins, minerals, and supplements for older adults.
Professional guidelines for nutrition assessment and intervention in older adults.
Information on federal nutrition programs and community resources for seniors.
Track Senior Nutrition & Dietary Needs with AveeCare
AveeCare's home care management software helps agencies track patient allergies, dietary restrictions, care plans, and nutritional documentation, making meal planning for seniors seamless across your care team.
No credit card required. No sales call needed. Try it yourself in minutes.
Disclaimer: This guide is intended for informational and educational purposes only and does not constitute medical or nutritional advice. Dietary plans should be developed in consultation with qualified healthcare providers and registered dietitians. Individual nutritional needs vary based on health conditions, medications, and personal factors. AveeCare provides home care management software and is not a healthcare or nutrition provider. Information is current as of April 2026 and may be subject to change.