Activities of Daily Living (ADL) Guide: Assessment, Documentation & Care Planning
A comprehensive activities of daily living checklist and ADL assessment resource for home care agencies. Includes an interactive Katz Index calculator, ADL chart reference, and evidence-based documentation guidance for care planning.
Published April 3, 2026 · 18 min read
What Are Activities of Daily Living?
Activities of daily living (ADLs) are the fundamental self-care tasks that a person must perform every day to maintain their health and well-being. First defined by physician Sidney Katz in 1963, the ADL framework has become the cornerstone of functional assessment in home care, geriatric medicine, and rehabilitation.
An ADL assessment measures a patient's ability to perform these essential tasks independently. When a person can no longer complete one or more activities of daily living without assistance, it signals the need for home care support. In the United States, ADL limitations are used as eligibility criteria for Medicare home health services, Medicaid waiver programs, long-term care insurance benefits, and Social Security disability determinations.
For home care agencies, accurate ADL documentation is not just a clinical necessity — it directly affects reimbursement rates, care plan development, staffing decisions, and regulatory compliance. Understanding how to properly assess, document, and track ADL performance is essential for delivering quality care and maintaining a sustainable agency. Our care plan documentation guide covers how to translate ADL findings into compliant, actionable care plans.

The 6 Basic Activities of Daily Living
The six basic ADLs are the core self-care activities evaluated in every ADL assessment. These activities are typically lost in a hierarchical order, with bathing independence usually declining first and feeding independence last. Understanding this hierarchy helps caregivers anticipate future care needs.
Bathing
ADL #1The ability to wash oneself, including getting in and out of a bathtub or shower.
Dressing
ADL #2Selecting appropriate clothing and putting it on, including fastening buttons and zippers.
Toileting
ADL #3Getting to and from the toilet, using it, and managing clothing before and after.
Transferring
ADL #4Moving in and out of a bed or chair without assistance.
Continence
ADL #5Maintaining control of bladder and bowel function.
Feeding
ADL #6The ability to feed oneself, including cutting food and bringing it to the mouth.
ADL Hierarchy of Loss
Research shows ADLs are typically lost in this order: bathing → dressing → toileting → transferring → continence → feeding. This pattern helps predict future care needs. If a patient is losing bathing independence, dressing difficulty may follow.
The 8 Instrumental Activities of Daily Living (IADLs)
Instrumental activities of daily living (IADLs) are the higher-level skills needed for independent community living. IADL deficits often appear before basic ADL decline and can be an early warning sign that a person needs home care services. The Lawton IADL Scale, developed in 1969, is the most widely used tool for assessing these capabilities. For patients with Alzheimer's disease or related conditions, IADL decline is often the earliest functional change -- our Alzheimer's home care guide explores how cognitive decline maps to ADL loss.
Managing Finances
Paying bills, managing bank accounts, handling budgets, and understanding financial documents.
Transportation
Driving, arranging rides, using public transit, or navigating ride-share services.
Shopping
Planning and purchasing groceries, clothing, and household necessities.
Meal Preparation
Planning, preparing, and serving meals, including operating kitchen appliances safely.
Housekeeping
Maintaining a clean home including vacuuming, dishes, laundry, and general tidying.
Medication Management
Taking medications in the correct dose at the correct time, managing refills.
Using Telephone
Making and receiving calls, looking up numbers, dialing, and carrying on a conversation.
Laundry
Sorting, washing, drying, folding, and putting away clothes.
ADL & IADL Assessment Tool
Rate the patient's level of independence for each activity of daily living. This assessment covers all 6 basic ADLs and 8 IADLs to provide a comprehensive functional profile.
Basic ADLs (Activities of Daily Living)
Rate each activity: 0 = Fully Dependent, 1 = Needs Some Help, 2 = Independent
Instrumental ADLs (IADLs)
Rate each activity: 0 = Unable, 1 = Needs Help, 2 = Independent
ADL Assessment Scales Comparison
Several validated ADL assessment scales are used in home care settings. Choosing the right scale depends on the purpose of the assessment, the patient population, and regulatory requirements. Below is an ADL chart comparing the three most widely used tools.
Katz Index of Independence
Developed 1963Barthel Index
Developed 1965Lawton IADL Scale
Developed 1969Katz Index of Independence Calculator
The Katz Index evaluates whether a patient can perform each of the 6 basic activities of daily living independently. Check each ADL the patient can perform without human assistance.
Katz Index Score
0/6Severe Impairment (Grade F-G)
Patient is dependent in most or all ADLs. Requires extensive daily care, possibly 24-hour supervision.
ADL Documentation Best Practices
Thorough ADL documentation is essential for proper care planning, reimbursement, and regulatory compliance. The activities of daily living checklist you document must paint a clear picture of what the patient can and cannot do, and what level of assistance is required for each task.
Be Specific, Not General
Instead of writing "patient needs help bathing," document the specific aspects: "Patient requires standby assistance for tub transfers and physical assistance washing lower extremities and back. Can wash face, upper body, and hair independently."
Document the Why
Record why the patient needs assistance. "Patient unable to dress lower body independently due to limited range of motion in right hip following total hip replacement 3 weeks ago" is far more informative than "patient needs help dressing."
Record Time and Frequency
Note how often and for how long assistance is needed. "Patient requires 15 minutes of hands-on assistance for morning bathing, 7 days per week" supports staffing decisions and reimbursement justification.
Track Changes Over Time
Document trends in ADL performance at every reassessment. Use consistent rating scales so improvements or declines are clearly measurable. Note any events that triggered changes (falls, hospitalizations, new medications).
Use Standardized Language
Use consistent terminology across all staff: "Independent," "Supervision," "Standby Assistance," "Minimal Assistance," "Moderate Assistance," "Maximal Assistance," "Total Dependence." Define these terms in your agency's documentation policy.
Connect ADLs to Goals
Link each ADL limitation to a specific, measurable care plan goal. For example, if the patient needs assistance with transferring, the goal might be "Patient will transfer from bed to wheelchair with standby assist only within 30 days."
Developing Care Plans from ADL Data
A well-conducted ADL assessment is only valuable if it drives a meaningful care plan. Here is how to translate ADL assessment findings into actionable, person-centered care plans that improve patient outcomes and satisfy regulatory requirements.
Identify Deficits from Assessment
List all ADLs and IADLs where the patient scored below independent. Prioritize deficits that affect safety (transferring, toileting) and health (feeding, medication management).
Set SMART Goals for Each Deficit
Create Specific, Measurable, Achievable, Relevant, Time-bound goals. Example: "Patient will independently transfer from bed to standing position with walker within 60 days of start of care."
Define Interventions
For each goal, specify the caregiver actions, equipment needed, safety precautions, and environmental modifications required. Include both restorative and maintenance interventions.
Determine Service Frequency
Use ADL scores to calculate how many hours per day and days per week of care are needed. Match staffing levels to the complexity and timing of care needs.
Schedule Reassessment
Set reassessment dates (typically every 60-90 days) to evaluate progress toward goals, adjust interventions, and modify service levels as the patient improves or declines.
Technology in ADL Tracking
Modern home care software has transformed how agencies track, document, and analyze ADL data. Digital tools reduce paperwork, improve accuracy, and enable data-driven care decisions that ultimately improve patient outcomes.
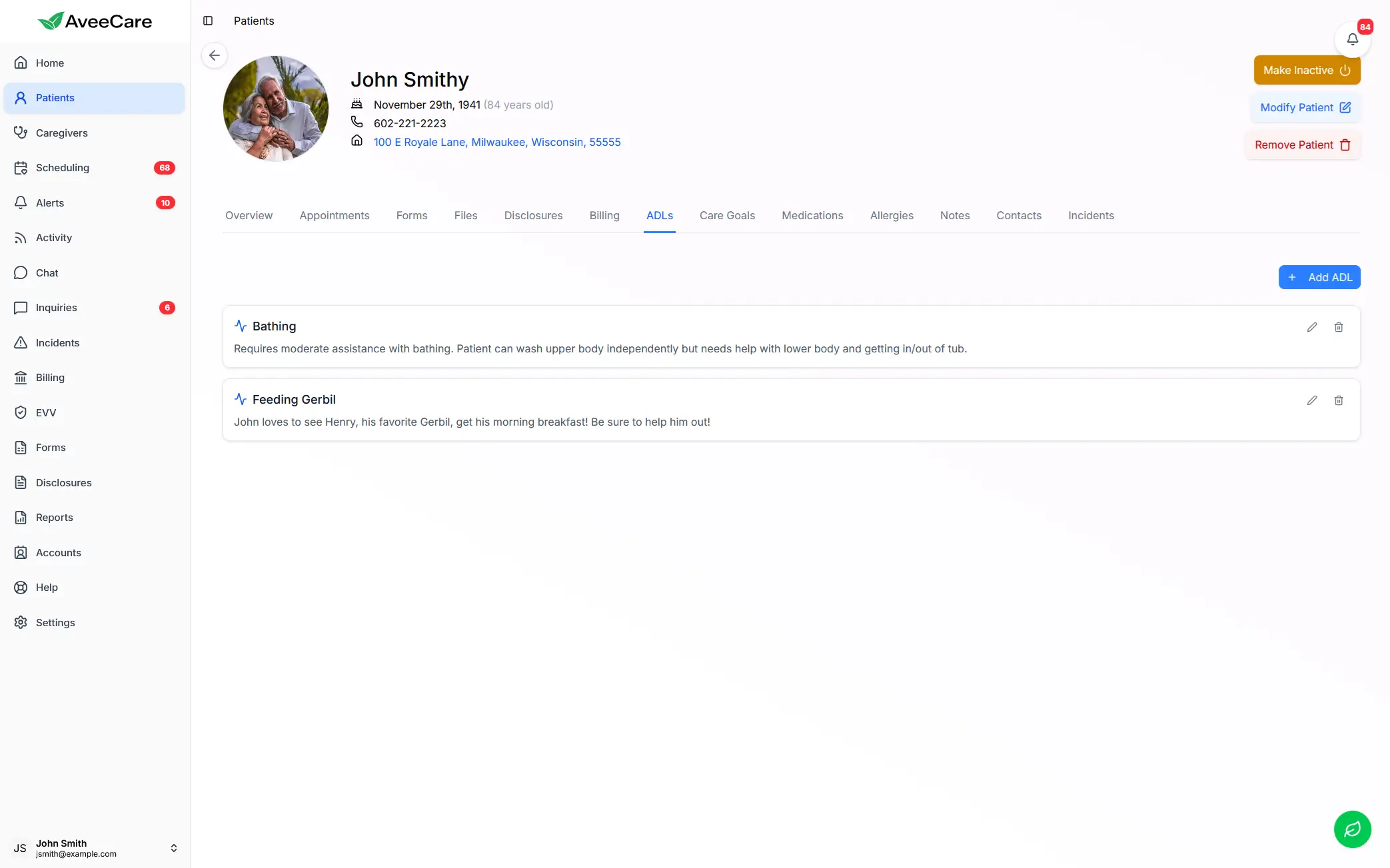
Digital ADL Assessments
Replace paper forms with standardized digital assessments that auto-calculate scores and flag changes from previous evaluations. Ensure consistency across all caregivers.
Automated Reassessment Alerts
Software can automatically remind staff when reassessments are due, preventing missed evaluations and keeping care plans current.
Trend Analysis & Reporting
Track ADL scores over time with visual charts and reports. Identify patients whose function is declining and intervene before a crisis.
Care Plan Integration
Link ADL assessment results directly to care plan goals and interventions, ensuring every documented deficit has a corresponding plan of action.
Frequently Asked Questions
Common questions about activities of daily living assessment and documentation.
Sources & References
Peer-reviewed research and authoritative sources cited in this guide.
Original paper defining the 6 basic activities of daily living and the Katz ADL Index.
Foundational paper establishing the 8 instrumental activities of daily living (IADL) scale.
Original publication of the Barthel Index, a weighted ADL assessment scale used in rehabilitation.
Official CMS guidance on ADL assessment items within the OASIS home health assessment instrument.
NIH resources on maintaining independence and the role of ADL support in aging at home.
Research on patterns of ADL decline in older adults, establishing the hierarchy of functional loss.
Streamline ADL Assessment & Documentation with AveeCare
AveeCare's home care management platform includes built-in ADL tracking with patient-specific default activities of daily living, automated reassessment reminders, and comprehensive care plan integration. Document ADL assessments digitally and generate compliance-ready reports — all from one platform.
Disclaimer
This guide is provided for informational and educational purposes only and does not constitute medical or clinical advice. Activities of daily living assessments should be conducted by qualified healthcare professionals using validated assessment tools appropriate for the patient population. ADL scores and assessment results should be interpreted in the context of each patient's overall clinical picture. Always follow your state's regulatory requirements, payer-specific documentation guidelines, and your agency's policies and procedures. Consult with appropriate licensed professionals for clinical decision-making.