Palliative Care at Home: A Complete Guide for Families & Agencies
Everything you need to understand about home palliative care, from symptom management and advance care planning to insurance coverage and when to transition to hospice. An evidence-based resource for home care agencies and families navigating end of life home care. For guidance on when palliative care shifts to end-of-life support, see our home health and hospice comparison guide, and for patients with cognitive decline alongside serious illness, explore our dementia care at home resource.

What Is Palliative Care at Home?
Palliative care at home is specialized medical care focused on providing relief from symptoms, pain, and stress of serious illness. The goal is to improve quality of life for both the patient and the family.
Palliative Care
Focuses on symptom relief and quality of life at any stage of serious illness. Can be provided alongside curative treatments. No life expectancy requirement.
Curative Care
Aims to cure the underlying disease through treatments like surgery, chemotherapy, or radiation. The primary goal is disease elimination or remission.
Hospice Care
A type of palliative care for patients with a terminal prognosis of 6 months or less. Curative treatment stops; the focus is entirely on comfort and dignity.
Palliative Care vs Hospice: Interactive Comparison
Understanding the difference between palliative care and hospice is essential for families and agencies. Use this interactive tool to compare them side by side across key dimensions.
Eligibility
Any serious illness, any stage. No life expectancy requirement.
Terminal diagnosis with prognosis of 6 months or less if disease runs its normal course.
Curative Treatment
Can be provided alongside curative treatments such as chemotherapy, radiation, or surgery.
Patient has chosen to stop curative treatments. Focus is entirely on comfort.
Goals of Care
Improve quality of life, manage symptoms, and support decision-making while pursuing treatment.
Maximize comfort, dignity, and quality of remaining life. Support for the dying process.
Care Team
Physician, nurse, social worker, chaplain. May coordinate with specialists.
Physician, nurse, aide, social worker, chaplain, volunteers, bereavement counselor.
Insurance Coverage
Medicare Part B, Medicaid, and most private insurance cover consultations and symptom management. Copays may apply.
Medicare Hospice Benefit (Part A) covers nearly all costs including medications, equipment, and respite care.
Duration
Can last months or years. No time limit as long as medical necessity exists.
Typically 6 months, but can be recertified if patient still meets criteria.
Setting
Home, hospital, outpatient clinic, or long-term care facility.
Primarily at home. Also in hospice facilities, hospitals, or nursing homes.
Bereavement Support
Not typically included, though social workers provide emotional support.
Bereavement support for family members for up to 13 months after death.
Who Benefits from Palliative Care at Home?
Palliative care at home is appropriate for patients with a wide range of serious illnesses. Early referral improves outcomes and quality of life for both patients and their families.
Cancer
All types and stages; palliative care alongside chemotherapy, radiation, or immunotherapy
Heart Failure
NYHA Class III-IV; managing dyspnea, fatigue, fluid retention, and end-stage planning
COPD
Advanced stages; breathlessness management, oxygen therapy, and anxiety reduction
Kidney Disease
Stage 4-5 CKD; symptom management for patients choosing conservative (non-dialysis) care
Dementia
Moderate to advanced; behavioral symptoms, caregiver support, and goals of care planning
ALS / Neurological
Progressive conditions; managing pain, breathing, mobility, and communication loss
Liver Disease
End-stage cirrhosis; managing ascites, encephalopathy, and transplant decisions
Multiple Chronic Conditions
Complex patients with 3+ serious conditions requiring coordinated symptom management
Frailty & Advanced Age
Older adults with functional decline, recurrent falls, and multiple geriatric syndromes
Symptom Management Reference
Effective palliative care symptom management uses both pharmacological and non-pharmacological approaches. Click on each symptom below to explore evidence-based management strategies for home palliative care.
Advance Care Planning & Goals of Care
Advance care planning is a cornerstone of palliative care at home. These conversations help ensure that the patient's wishes are known, documented, and honored throughout their illness.
Essential Documents
- Advance Directive / Living Will
Specifies treatment preferences for life-sustaining measures
- Healthcare Power of Attorney
Designates a decision-maker when patient cannot speak for themselves
- POLST / MOLST Form
Physician-signed orders for specific treatments (CPR, intubation, hospitalization)
- DNR / DNI Orders
Do Not Resuscitate and Do Not Intubate orders if desired
- HIPAA Authorization
Allows designated individuals to access medical information
Goals of Care Conversations
Goals of care conversations should happen early and be revisited as the illness progresses. Use these frameworks to guide the discussion:
- 1.Understand: "What is your understanding of your illness and where things stand?"
- 2.Values: "What matters most to you as you think about the future?"
- 3.Worries: "What are you most worried or afraid of?"
- 4.Tradeoffs: "How much are you willing to go through for the possibility of more time?"
- 5.Family: "How much do your family members know about your wishes?"
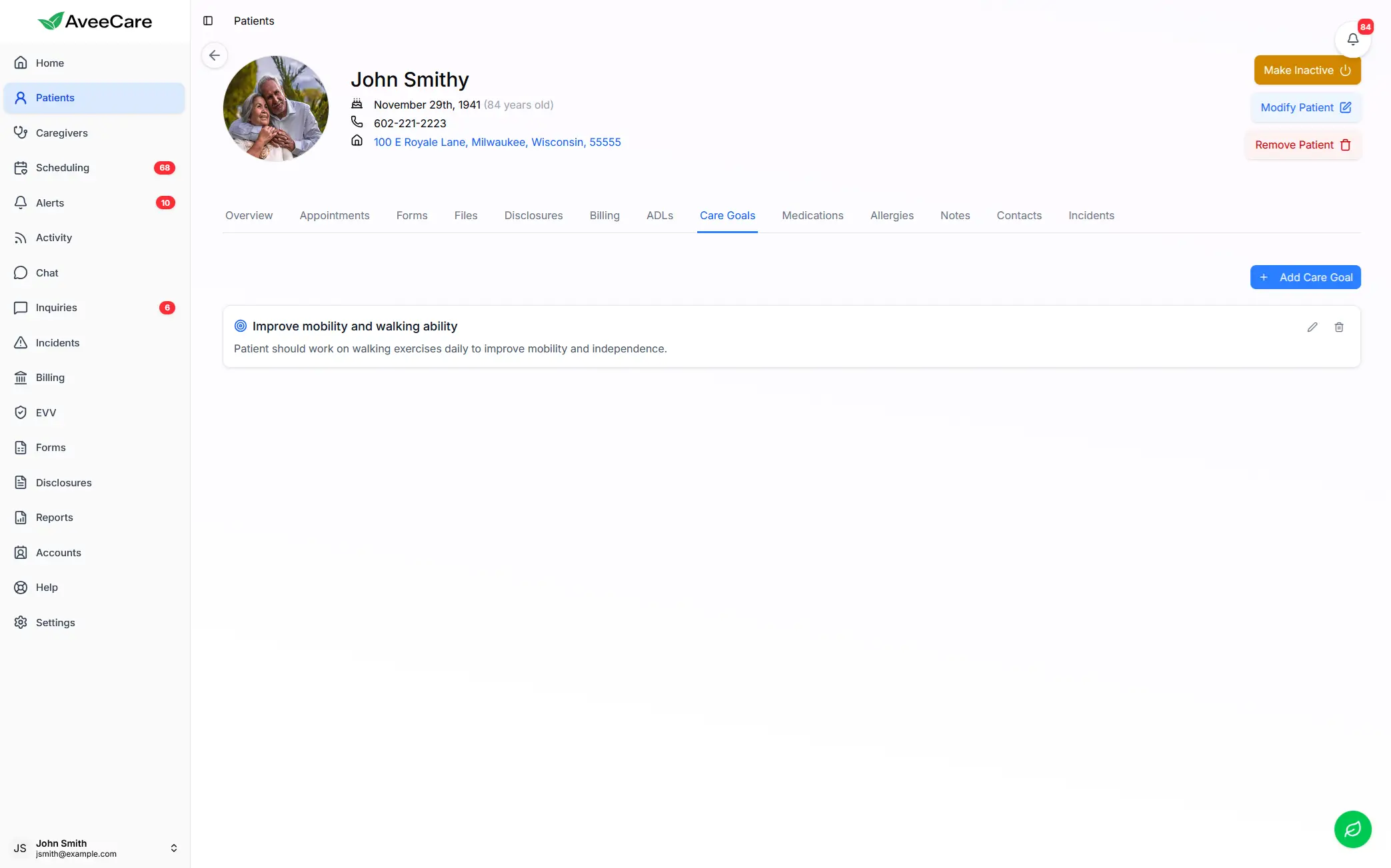
AveeCare's care goals tracking helps agencies document and monitor palliative care plans
The Palliative Care Team at Home
Home palliative care is delivered by an interdisciplinary team. Each member plays a specific role in addressing the physical, emotional, social, and spiritual needs of the patient and family.
Palliative Care Physician / NP
- Leads symptom management and medication adjustments
- Conducts goals of care conversations
- Coordinates with specialists and primary care
- Certifies and recertifies care plans
Registered Nurse
- Performs symptom assessments at each visit
- Educates patient and family on medications
- Provides wound care and IV management
- Monitors for changes in condition
Social Worker
- Facilitates advance care planning discussions
- Connects families with community resources
- Provides counseling and emotional support
- Assists with insurance and financial navigation
Chaplain / Spiritual Counselor
- Addresses spiritual and existential distress
- Supports patients of all faiths and backgrounds
- Facilitates legacy and meaning-making activities
- Provides presence and listening during difficult times
Home Health Aide
- Assists with ADLs: bathing, dressing, grooming
- Helps with mobility and transfers
- Prepares meals and assists with feeding
- Reports changes in condition to the nursing team
Bereavement Counselor
- Provides grief support to family members
- Facilitates support groups
- Identifies complicated grief reactions
- Connects families with ongoing resources
Insurance Coverage for Home Palliative Care
Understanding insurance coverage is critical for families and agencies providing palliative care at home. Coverage varies by payer, service type, and state regulations.
Medicare
- Part B covers physician consultations and symptom management
- Home health benefit covers skilled nursing and therapy services
- Part D covers prescription medications
- Hospice Benefit (Part A) covers comprehensive end-of-life care
- Copays and deductibles may apply for non-hospice palliative services
Medicaid
- Coverage varies significantly by state
- Most states cover physician palliative care consultations
- Home and community-based waivers may cover additional services
- Many states offer concurrent care for children (curative + hospice)
- Contact your state Medicaid office for specific coverage details
Private Insurance
- Most plans cover palliative care consultations as specialist visits
- Coverage depends on plan type, network, and specific services
- Prior authorization may be required for some services
- Check policy for home health benefits and limitations
- Many plans now include palliative care as a covered benefit
Veterans Affairs (VA)
- VA covers palliative care for enrolled veterans
- Home-Based Primary Care (HBPC) provides in-home services
- VA hospice can be provided at home, in VA facilities, or via community partnerships
- No copays for hospice or palliative care services
- Aid and Attendance benefits may supplement home care costs
When to Transition from Palliative Care to Hospice
Recognizing when a patient may benefit from hospice care is an important part of end of life home care. The transition should be guided by the patient's prognosis, goals, and wishes.
Signs That Hospice May Be Appropriate
Steps for a Smooth Transition
Initiate the Conversation
Discuss hospice with the patient and family as a natural progression of care, not a giving up. Frame hospice as choosing comfort and quality.
Obtain Physician Certification
Two physicians must certify that the patient has a terminal prognosis of 6 months or less for Medicare Hospice Benefit eligibility.
Choose a Hospice Provider
Research local hospice agencies. Consider their reputation, available services, response times, and whether they provide 24/7 on-call support.
Coordinate Care Transfer
Ensure complete medical records transfer, medication reconciliation, and clear handoff between the palliative care team and hospice team.
Support the Family
Provide emotional support, explain what to expect, and ensure the family understands that hospice can be revoked if the patient improves or changes their mind.
Frequently Asked Questions
Common questions about palliative care at home, hospice, and end of life home care.
Sources & References
This guide draws on peer-reviewed research and authoritative clinical guidelines for palliative care at home.
National data on palliative and hospice care utilization, quality metrics, and best practices.
Clinical guidelines, training resources, and program development tools for palliative care.
Official Medicare coverage information for hospice and palliative care services.
Research-based palliative care resources and end-of-life science.
Global guidelines for symptom management including the WHO analgesic ladder for pain.
Deliver Compassionate Palliative Care with AveeCare
AveeCare's home care management software helps agencies coordinate palliative care at home with care goal tracking, symptom documentation, caregiver scheduling, family communication, and real-time alerts, all in one simple platform.
No credit card required. No sales call needed. Try it yourself in minutes.
Disclaimer: This guide is intended for informational and educational purposes only and does not constitute medical advice. Palliative care decisions should be made in consultation with qualified healthcare providers. Individual patient needs vary, and all treatment plans should be tailored to the specific clinical situation. AveeCare provides home care management software and is not a healthcare provider. Always consult with a physician or palliative care specialist for medical guidance. Information is current as of April 2026 and may be subject to change.