Value-Based Care in Home Health: HHVBP Model, Metrics & Strategies
The shift from volume to value is transforming home health care. Under the HHVBP model, Medicare now adjusts payments by up to 5% based on your quality scores. This guide explains every quality metric, shows you how payment adjustments work, and gives you proven strategies to improve your performance -- with interactive tools to estimate your payment impact and assess your readiness for value-based care in home health.
What Is Value-Based Care in Home Health?
Value-based care in home health represents a fundamental shift in how Medicare pays home health agencies. Rather than paying a flat rate for each episode of care regardless of results, value-based care in home health ties a portion of Medicare reimbursement to measurable quality outcomes. Agencies that deliver better patient outcomes, higher patient satisfaction, and lower hospitalization rates earn payment bonuses, while underperformers face reductions.
This model, formalized through the Home Health Value-Based Purchasing (HHVBP) program, affects every Medicare-certified home health agency in the United States. In 2026, the payment adjustment range is plus or minus 5%, meaning the difference between top and bottom performers can be a 10 percentage point swing in Medicare revenue -- a significant financial impact for agencies of any size. Agencies running dual service lines should also see our home health and hospice software guide, and improving patient satisfaction is one of the most direct ways to boost your HHVBP score.
The HHVBP Model: How It Works
The Home Health Value-Based Purchasing model was first piloted by CMS in 2016 across nine randomly selected states. After demonstrating quality improvements and Medicare savings of approximately $141 million during the pilot period, CMS expanded the HHVBP model nationally starting January 1, 2023. Under home health value-based purchasing, every Medicare-certified home health agency is now evaluated on a set of quality measures that determine their payment adjustment.
Timeline
HHVBP pilot in 9 states demonstrated quality improvements and $141M in Medicare savings
National expansion to all 50 states and territories; CY2023 performance data collection begins
First payment adjustments under national expansion applied (based on CY2023 performance)
Payment adjustments reach full +/-5% range; CY2024 performance data drives current adjustments
Scoring Components
Your Total Performance Score (TPS) is calculated from two components for each measure:
Achievement Score
Compares your current performance to national benchmarks. Higher achievement relative to the benchmark earns more points.
Improvement Score
Measures your improvement over your own baseline period. Even agencies below benchmarks can earn points by demonstrating significant improvement.
CMS uses the higher of the two scores for each measure, giving agencies credit for both absolute performance and improvement trajectory.
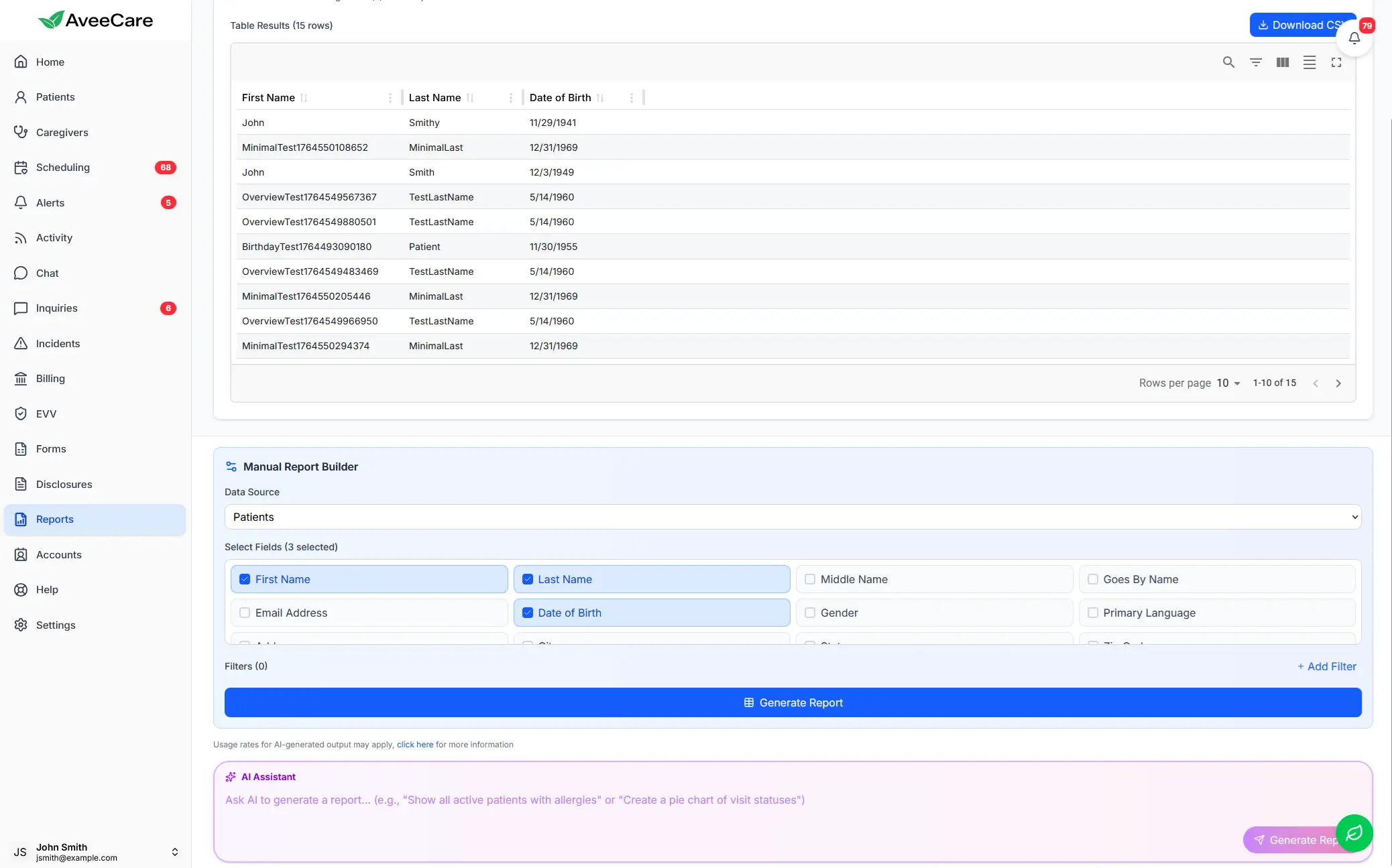
AveeCare helps agencies track quality metrics with AI-powered custom reports
Quality Measures and Benchmarks
Understanding the quality metrics used in home health value-based purchasing is essential for improving your performance. These measures fall into three categories: OASIS-based outcomes, HHCAHPS patient experience, and claims-based utilization. Each quality metric for home health carries a specific weight in the overall scoring, with claims-based measures having the largest impact on your payment adjustment.
Improvement in Ambulation
Percentage of patients showing improvement in walking or moving around
Improvement in Bathing
Percentage of patients showing improvement in bathing ability
Improvement in Bed Transferring
Percentage of patients improving ability to transfer in and out of bed
Improvement in Dyspnea
Percentage of patients showing improvement in shortness of breath
Improvement in Oral Medication Management
Percentage of patients improving ability to manage oral medications
Overall Patient Rating (9-10)
Percentage of patients rating agency 9 or 10 out of 10
Would Recommend Agency
Percentage of patients who would definitely recommend agency
Communication Quality
How well providers communicated with patients
Acute Care Hospitalization Rate
Unplanned hospital admissions during home health episode
ED Use Without Hospitalization
Emergency department visits that did not result in admission
HHVBP Payment Adjustment Calculator
Enter your quality scores below to estimate your payment adjustment under value-based care in home health. This calculator models the HHVBP scoring methodology to project your approximate payment impact.
Higher is better | Benchmark: 68%
Higher is better | Benchmark: 72%
Higher is better | Benchmark: 65%
Higher is better | Benchmark: 73%
Higher is better | Benchmark: 55%
Higher is better | Benchmark: 84%
Higher is better | Benchmark: 79%
Higher is better | Benchmark: 87%
Lower is better | Benchmark: 16%
Lower is better | Benchmark: 12%
Strategies to Improve HHVBP Performance
Improving your performance under the HHVBP model requires a multi-faceted approach that touches every aspect of your home health operations. Here are the proven strategies that high-performing agencies use to achieve top quality metrics in home health.
OASIS Assessment Accuracy
- Implement inter-rater reliability testing for all clinicians
- Conduct monthly OASIS accuracy audits on a random sample
- Provide real-time OASIS guidance tools at the point of care
- Train clinicians on common OASIS scoring errors and their impact on quality measures
Hospitalization Prevention
- Frontload nursing visits in the first 48-72 hours of each episode
- Implement medication reconciliation at start of care
- Establish telehealth or remote monitoring for high-risk patients
- Create rapid response protocols for early signs of decline
Patient Experience (HHCAHPS)
- Train all staff on communication best practices and empathy
- Set clear expectations during the first visit about the plan of care
- Implement consistent caregiver assignment when possible
- Follow up after discharge to address any concerns proactively
Data-Driven Quality Management
- Track quality measure performance monthly against national benchmarks
- Identify clinicians or teams with outlier performance for targeted coaching
- Use predictive analytics to identify patients at highest risk for hospitalization
- Benchmark against top-decile performers and set incremental improvement targets
Clinical Outcome Improvement
- Implement evidence-based care pathways for common conditions
- Focus on patient and family education for self-management
- Coordinate with physicians on medication management and functional goals
- Use standardized outcome measurement tools beyond OASIS
Staff Engagement & Training
- Link quality performance to staff recognition and incentives
- Provide quarterly quality performance feedback to individual clinicians
- Invest in ongoing education on value-based care in home health principles
- Create quality improvement committees with frontline staff participation

Value-Based Care Readiness Assessment
Evaluate how prepared your agency is for success under the HHVBP model. Answer these questions to identify your strengths and areas for improvement in home health value-based purchasing readiness.
1. How accurately and consistently do your clinicians complete OASIS assessments?
2. Does your agency currently track and monitor quality measure performance?
3. How does your agency approach hospitalization prevention?
4. What patient experience initiatives does your agency have?
5. How does your agency use data and analytics for clinical decision-making?
6. Does your home health software support quality reporting and benchmarking?
Technology Tools for Value-Based Care in Home Health
Succeeding under the HHVBP model requires technology that goes beyond basic scheduling and billing. Home health agencies need software that supports quality tracking, clinical decision support, outcome measurement, and analytics -- all integrated into daily workflows so quality improvement is continuous rather than reactive.
Quality Dashboards
Real-time tracking of all HHVBP quality measures against national benchmarks with drill-down capabilities
AI Analytics
Machine learning models that predict hospitalization risk and identify patients needing intervention
OASIS Guidance
Built-in OASIS assessment tools with accuracy checks and real-time guidance at the point of care
Outcome Tracking
Automated tracking of patient functional outcomes tied directly to quality measure reporting
Staff Scorecards
Individual clinician performance dashboards showing quality metrics and improvement trends
Benchmarking
Compare your performance against state and national averages with automated gap analysis
Frequently Asked Questions
Sources & References
Track Your Quality Metrics with AveeCare
AveeCare gives home health agencies the tools to succeed under value-based care. AI-powered analytics, custom quality reports, and integrated outcome tracking help you monitor HHVBP performance and drive continuous improvement -- all with transparent pricing and no mandatory demos.
Trusted by home care agencies across all 50 states. Private pay, Medicare, and long-term care insurance billing included.
Disclaimer: This article is for informational purposes only and does not constitute legal, medical, or financial advice. HHVBP payment adjustment estimates provided by the calculator are approximate and may not reflect actual CMS calculations. Quality measure benchmarks are based on publicly available CMS data and may change. Always consult the latest CMS guidelines and a qualified healthcare consultant for compliance decisions. Published April 3, 2026.