Home Care in Rural Communities: Challenges, Solutions & Strategies
Rural home care agencies face unique obstacles from caregiver shortages to geographic coverage gaps. This guide provides data-driven strategies, interactive tools, and federal resources to help your agency deliver exceptional care in rural areas.
Published April 3, 2026 · 18 min read
Rural Home Care: The Landscape
Nearly 46 million Americans live in rural areas, representing about 14% of the U.S. population across 97% of the nation's land area. Rural populations skew significantly older: 17.5% of rural residents are aged 65 or older, compared to 13.8% in urban areas, according to the U.S. Census Bureau. This demographic reality creates outsized demand for home care services in rural communities.
Yet rural home care agencies face a stark supply-demand imbalance. HRSA data shows that over 60% of Health Professional Shortage Areas (HPSAs) are in rural regions. The National Rural Health Association reports that rural areas have 43 physicians per 100,000 people compared to 134 per 100,000 in urban areas, meaning home care serves as a critical bridge for medical and non-medical support. For home care in rural areas, agencies must overcome geographic, workforce, and infrastructure challenges that their urban counterparts rarely face. These staffing gaps mirror the broader home care workforce shortage, and our staffing and recruitment guide offers strategies that apply to rural agencies as well.
The rural caregiver shortage is particularly acute. While the BLS projects 22% growth in home health and personal care aide demand through 2032, rural agencies consistently report that recruiting qualified caregivers is their number one operational challenge. Median home care aide wages in rural counties average $2-3 per hour less than urban and suburban rates, making it even harder to attract and retain workers in areas where every caregiver matters.

Rural caregivers often provide care across vast geographic areas, bringing essential services to communities underserved by traditional healthcare infrastructure.
Rural Agency Challenge Assessment
Rate each rural home care challenge based on how severely it affects your agency. You will receive prioritized solutions tailored to your biggest obstacles for delivering home care in rural areas.
Caregiver Shortage
Difficulty recruiting and retaining caregivers due to smaller population and limited labor pool.
Travel Distance
Long driving distances between client homes that reduce billable hours and increase costs.
Limited Connectivity
Poor broadband and cellular coverage affecting telehealth, documentation, and communication.
Low Reimbursement
Payment rates that do not account for higher travel costs and lower client density.
Training Access
Limited access to in-person continuing education and specialized training programs.
Referral Networks
Fewer referral sources due to limited healthcare infrastructure and provider shortages.
Caregiver Isolation
Caregivers working alone in remote areas without peer support or immediate backup.
Emergency Response
Longer emergency response times requiring more advanced caregiver first-response capabilities.
Travel Cost Calculator
Estimate your agency's monthly travel costs and see how route optimization can reduce mileage expenses in your rural home care service area.
IRS Standard Mileage Rate (2026)
$0.70/mile
Monthly Mileage Cost
Monthly Travel Hours
Of Each Day Driving
With Route Optimization (est. 25% reduction)
Optimized Monthly Cost
$7,277
Monthly Savings
$2,426
Annual Savings
$29,106
Scheduling Efficiency for Large Service Areas
Geographic coverage is one of the defining challenges of rural home care. These strategies help agencies manage large territories while maximizing billable hours and minimizing windshield time.
Geographic Client Clustering
Group clients into geographic zones and assign caregivers to zones near their homes. This hub-and-spoke model reduces daily travel and allows caregivers to build deeper relationships within their community cluster.
Optimized Visit Sequencing
Schedule visits in geographic order rather than chronological order when possible. Use route optimization software to calculate the most efficient visit sequence for each caregiver each day.
Community Health Worker Integration
Train and deploy community health workers (CHWs) who already live in rural communities. CHWs provide culturally appropriate care, have existing community relationships, and eliminate long commutes.
Telehealth-Augmented Care
Use virtual check-ins for stable clients who do not need hands-on care at every visit. Telehealth can replace one in three routine visits for appropriate clients, dramatically reducing travel.
Rural Hospital Partnerships
Partner with Critical Access Hospitals (CAHs) and Federally Qualified Health Centers (FQHCs) for referral pipelines and shared resources. Rural hospitals often have underutilized space for caregiver staging.
Creative Staffing Models
Implement live-in care for remote clients when daily visits are impractical. Offer extended shift options (10-12 hours) to reduce the number of daily trips. Create weekend-only and float positions for flexible coverage.
Real-Time Map Tracking for Rural Coverage
See where your caregivers are and manage geographic coverage in real time
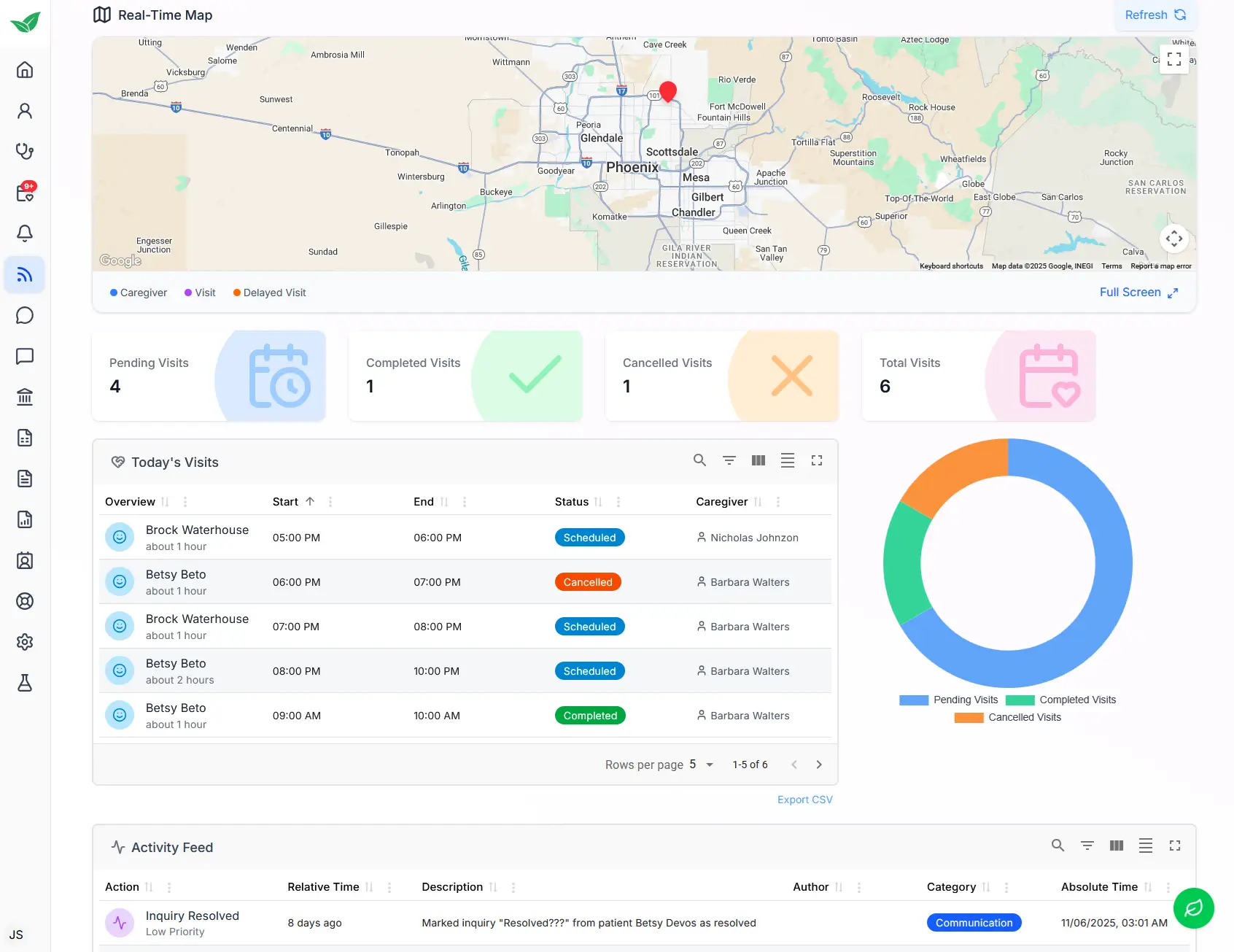
Rural Connectivity Solutions Comparison
Approximately 24% of rural Americans lack broadband access, according to the FCC. Compare connectivity options for your rural home care operations. Click any card to see detailed pros and cons.
Satellite Internet
Fixed Wireless
Cellular Hotspot
DSL (Extended Reach)
Offline-First Best Practices for Rural Home Care
- Use home care software with offline mode that syncs automatically when connectivity returns
- Pre-download care plans, medication lists, and visit notes before heading to remote areas
- Carry a cellular hotspot as a backup connectivity source during visits
- Establish text-based communication protocols for areas with voice-only cellular coverage
- Document visit times and tasks on paper as a fallback, then enter electronically when connectivity is available
Federal & State Funding for Rural Home Care
Multiple federal programs provide grants, loans, and enhanced reimbursement for healthcare providers serving rural communities. Here are the key funding sources every rural home care agency should know.
HRSA Federal Office of Rural Health Policy
Awards grants for rural healthcare workforce development, telehealth expansion, network development, and community-based outreach. Competitive grant cycles typically open annually.
Eligibility: Rural healthcare organizations, networks, and state offices of rural health
USDA Rural Development
Community Facilities Direct Loan and Grant Program funds essential community facilities including healthcare infrastructure. Distance Learning and Telemedicine grants support technology adoption.
Eligibility: Rural areas with population under 20,000
FCC Rural Health Care Program
Provides subsidized broadband connectivity for rural healthcare providers. The Healthcare Connect Fund covers up to 65% of broadband costs for eligible facilities.
Eligibility: Nonprofit and public healthcare providers in rural areas
Medicare HPSA Bonus
Physicians and certain practitioners in Health Professional Shortage Areas receive a 10% bonus on Medicare payments. Home health agencies in HPSAs may qualify for additional adjustments.
Eligibility: Providers serving designated HPSA areas
State Offices of Rural Health
Each state has an Office of Rural Health that administers federal pass-through grants and state-specific programs for rural healthcare workforce recruitment, retention, and infrastructure.
Eligibility: Varies by state program
National Health Service Corps
Provides student loan repayment for healthcare professionals who commit to working in underserved areas for at least two years. Includes nurses and certain allied health professionals.
Eligibility: Licensed healthcare providers in approved NHSC sites
Telehealth Adoption in Rural Home Care
Telehealth is transforming rural home health care by enabling more frequent check-ins, reducing unnecessary emergency department visits, and connecting rural patients with specialists. Here is what the evidence shows.
Reduction in rural ED visits with telehealth monitoring
Source: HRSA Telehealth Research
Of rural patients report satisfaction with telehealth home care
Source: National Rural Health Association
Of rural home health agencies now use telehealth
Source: NAHC 2025 Survey
Average savings per avoided rural ED transport
Source: CMS Innovation Center
For rural home care agencies, telehealth is not a replacement for in-person visits but a powerful supplement. The most effective model combines regular hands-on visits with virtual check-ins between appointments. This approach allows caregivers to monitor clients more frequently without the travel burden that makes rural care so expensive.
Key telehealth use cases for rural home care include medication adherence checks, vital sign monitoring for chronic conditions, caregiver supervision and support, family care conferences with out-of-town relatives, and mental health check-ins for isolated rural seniors. Agencies that adopt telehealth report 15-25% reductions in travel-related costs while maintaining or improving client outcomes.
Frequently Asked Questions
Data Sources
The statistics, benchmarks, and program details in this guide are drawn from the following authoritative sources.
Health Resources and Services Administration
Federal Office of Rural Health Policy data, HPSA designations, and rural health workforce reports. Telehealth research and grant program data.
U.S. Department of Agriculture
Rural Development program data, Community Facilities funding reports, and rural demographics from the Economic Research Service.
National Rural Health Association
Rural health policy briefs, workforce studies, telehealth adoption surveys, and annual rural health conference research.
Centers for Medicare & Medicaid Services
Rural health payment policies, HPSA bonus calculations, Innovation Center rural health models, and home health reimbursement data.
Federal Communications Commission
Broadband deployment reports, Rural Health Care Program data, and rural connectivity coverage maps.
U.S. Census Bureau
Rural population demographics, aging population projections, and American Community Survey data for rural areas.
Built for Rural Home Care
AveeCare's home care software is designed to address the unique challenges of rural agencies. Real-time GPS tracking, route-optimized scheduling, offline-capable documentation, and built-in messaging keep your caregivers connected and efficient across vast service areas.
- Real-time GPS map tracking for rural caregiver coverage visibility
- Route-optimized scheduling that clusters visits geographically
- Mobile-first documentation with offline capability for low-connectivity areas
- HIPAA-compliant messaging to combat rural caregiver isolation
- Cloud-based access from anywhere with no on-premise servers required
Sources & Disclaimer
Statistics and program details in this guide are compiled from publicly available data published by HRSA, USDA, the National Rural Health Association, CMS, FCC, and the U.S. Census Bureau. Specific figures may vary by state, county, and program cycle.
The travel cost calculator provides estimates based on average mileage rates and driving patterns. Actual costs will vary based on geography, fuel prices, vehicle type, and local conditions. This guide is for educational purposes and does not constitute financial, legal, or clinical advice.
Last updated: April 2026. AveeCare reviews and updates resource guides annually.