Home Care Patient Rights
Patient rights in home care are federally and state-mandated protections that every agency must understand, document, and uphold. This guide provides an interactive Bill of Rights template builder, compliance checklist, and comprehensive coverage of the home care bill of rights requirements every agency must meet. Understanding client rights in home care is essential for compliance and quality care.
Federal Patient Rights Requirements
The federal framework for patient rights in home care is established primarily through the CMS Conditions of Participation (42 CFR Part 484) for Medicare-certified agencies, HIPAA for privacy protections, the Americans with Disabilities Act for accessibility, and Title VI of the Civil Rights Act for non-discrimination. Even non-Medicare agencies must comply with many of these provisions through state licensing laws that incorporate federal standards. Patient rights also intersect with your agency's informed consent procedures and abuse and neglect reporting obligations.
CMS Conditions of Participation governing patient rights for home health agencies
HIPAA Privacy Rule protecting confidentiality of patient health information
All 50 states have patient rights requirements in home care licensing laws
CMS Conditions of Participation
Section 484.50 requires Medicare-certified HHAs to inform patients of their rights, provide written notice, and protect patients from abuse and exploitation. These are minimum standards enforced through federal surveys.
HIPAA Privacy Rule
Requires agencies to provide a Notice of Privacy Practices, obtain authorization before disclosing PHI, and grant patients the right to access and amend their records. Applies to all agencies that transmit health information electronically.
Americans with Disabilities Act
Prohibits discrimination against individuals with disabilities and requires reasonable accommodations in communication and care delivery. Affects accessible formats for rights documents and interpreter services.
Patient Self-Determination Act
Requires agencies to inform patients of their right to create advance directives (living wills, healthcare powers of attorney) and to document whether the patient has executed an advance directive.
State Patient Bill of Rights Requirements
Every state has its own home care licensing regulations that include patient rights provisions. State laws often exceed federal minimums by adding requirements specific to non-medical home care, personal care, and companion care services. Here are the common elements found across state home care bill of rights requirements.
Patient Bill of Rights Template Builder
Select the patient rights applicable to your agency to generate a customizable Bill of Rights document. Required items are pre-selected based on federal and common state requirements. Copy the generated document to customize further for your agency. This tool helps you build a comprehensive home care client rights document.
Select Rights to Include
Your Agency Name
Patient Bill of Rights
Dignity & Respect
- The right to be treated with courtesy, dignity, and respect at all times.
- The right to receive care without discrimination based on race, color, religion, national origin, sex, age, disability, sexual orientation, or source of payment.
Information
- The right to be informed of all services available, including charges and payment methods, before care begins.
- The right to receive a written notice of rights and responsibilities before or at the start of services.
- The right to be informed of the name, credentials, and role of all personnel providing care.
Participation
- The right to participate in the development and revision of the care plan.
- The right to be informed in advance of any changes in care, treatment, or services.
Choice & Refusal
- The right to refuse treatment or services without fear of retribution or discrimination.
- The right to choose a healthcare provider and to change providers at any time.
Privacy & Confidentiality
- The right to confidentiality of medical records and personal information under HIPAA.
- The right to privacy during care activities and in personal communications.
Safety
- The right to receive care in a safe setting free from abuse, neglect, and exploitation.
- The right to have property and possessions treated with respect and free from theft.
Grievance
- The right to voice grievances and complaints without fear of retaliation.
- The right to be informed of the agency's complaint resolution process and the state complaint hotline.
Financial
- The right to be informed of expected charges, payment sources, and any financial liability before services begin.
Advance Directives
- The right to formulate advance directives and have the agency comply with them.
Access
- The right to access personal medical records within a reasonable timeframe upon request.
Effective Date: April 2026
Patient/Authorized Representative Signature
Date: _______________
Agency Representative Signature
Date: _______________
Right to Information
Patients have the right to receive comprehensive information about their care before it begins. This is one of the most fundamental patient rights in home care and is a requirement under both federal and state law. Agencies must provide this information in a manner the patient can understand, which may require translated documents or interpreter services.
Names, credentials, and contact information for all caregivers assigned
Patients should know who will be entering their home and be able to verify their qualifications.
Complete description of services to be provided and schedule of visits
The care plan should be explained in plain language, not medical terminology.
All charges, fees, and billing practices explained in writing before services begin
No surprise billing. Patients must understand their financial obligations clearly.
Agency ownership, licensure status, and contact information
Patients can verify the agency is properly licensed through their state health department.
How to contact the agency 24/7 for urgent issues or schedule changes
Emergency contact procedures must be provided in writing and be easily accessible.
Right to Choose & Refuse Services
The right to refuse treatment is one of the most fundamental patient rights and responsibilities in home care. Patients have the absolute right to accept or reject any proposed service, treatment, or caregiver. Agencies must respect refusals without retaliation, discrimination, or withdrawal of other services. Refusals must be documented with the patient's stated reason and the potential consequences explained.
Right to Choose
- Choose or change their home care provider at any time
- Request a specific caregiver or request a caregiver change
- Participate in selecting the services they receive
- Access a second opinion from another provider
Right to Refuse
- Refuse any specific service or treatment
- Refuse a specific caregiver
- Refuse to participate in research or experimental treatments
- Discontinue services at any time
Privacy & Confidentiality Under HIPAA
HIPAA protections are a critical component of patient rights in home care. Home care agencies are covered entities under HIPAA and must safeguard all protected health information (PHI). The home setting creates unique privacy challenges that agencies must address through training, policies, and technology safeguards.
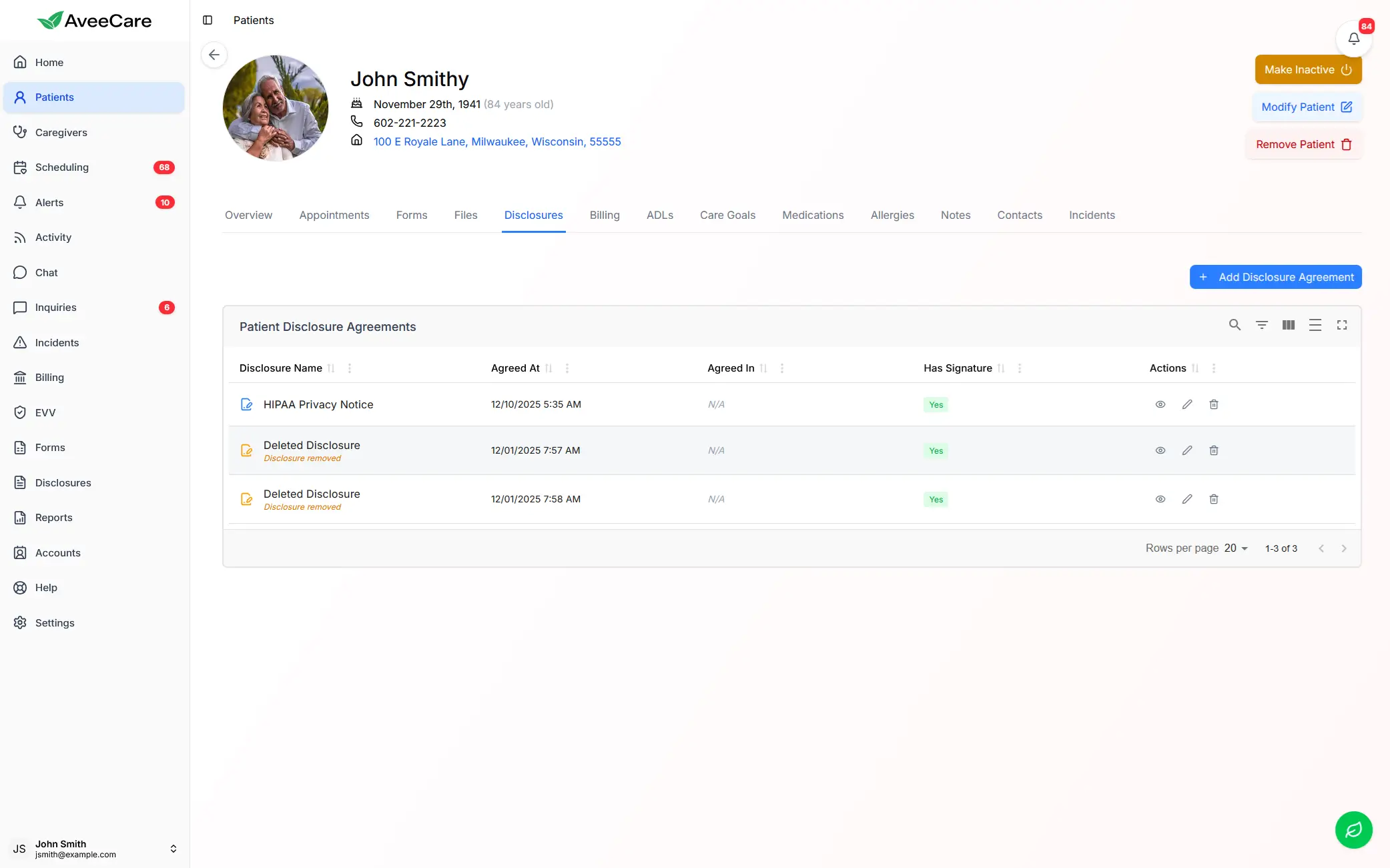
Notice of Privacy Practices
Agencies must provide a written NPP at intake explaining how PHI is used, disclosed, and protected. Patients must acknowledge receipt. The NPP must describe the patient's rights regarding their health information.
Minimum Necessary Standard
Caregivers should only access the PHI necessary to perform their assigned duties. A companion care aide does not need access to detailed medical histories. Access controls in home care software should enforce this.
Right to Access Records
Under HIPAA 45 CFR 164.524, patients have the right to inspect and obtain copies of their medical records within 30 days of a request. Agencies may charge a reasonable cost-based fee for copies.
Right to Amend Records
Patients can request amendments to their records if they believe information is inaccurate. Agencies have 60 days to respond and may deny amendments only with specific justification.
Patient Rights Compliance Checklist
Check off each item to track your agency's compliance with home care client rights requirements. This checklist covers documentation, language access, privacy, grievance procedures, and staff training obligations.
Patient Rights Compliance
0% CompleteDocumentation
Language Access
Privacy
Grievance
Training
Advance Directives
Financial
Participation
Civil Rights
Accessibility
Safety
Establishing Grievance Procedures
A robust grievance procedure is both a legal requirement and a quality improvement tool. Patient rights and responsibilities in home care include the right to voice complaints without fear of retaliation. Your grievance procedure should be accessible, timely, and transparent.
Step 1: Intake & Acknowledgment
Accept complaints verbally, in writing, or electronically. Acknowledge receipt within 24 hours with a written confirmation that includes a case number and expected timeline for resolution.
Step 2: Investigation
Assign an investigator who was not involved in the complaint. Interview all parties, review documentation, and gather facts within 5-10 business days. Document every step of the investigation.
Step 3: Resolution & Communication
Communicate findings and resolution to the complainant within 30 days. Explain corrective actions taken. If the complaint is substantiated, implement immediate remedial measures.
Step 4: Appeal Process
Provide a written appeal process if the complainant is unsatisfied. Include information on how to contact the state health department complaint line and any applicable ombudsman programs.
Step 5: Documentation & Trend Analysis
Maintain a grievance log with dates, categories, and outcomes. Review quarterly for patterns that indicate systemic issues requiring policy or training changes.
Cultural Considerations & Language Access
Title VI of the Civil Rights Act and CMS requirements mandate that home care agencies provide meaningful access to services for patients with limited English proficiency (LEP). Cultural competency goes beyond language to include understanding and respecting diverse health beliefs, practices, and communication styles.

Translate Vital Documents
Translate the Patient Bill of Rights, Notice of Privacy Practices, consent forms, and grievance procedures into languages spoken by 5% or more of your patient population.
Qualified Interpreters
Use qualified medical interpreters, not family members or bilingual staff without interpreter training. Telephonic interpreter services are acceptable and often cost-effective.
Cultural Competency Training
Train all staff on cultural sensitivity, health beliefs of common patient populations, dietary and religious considerations, and effective cross-cultural communication.
Document Language Preferences
Record each patient's preferred language and communication needs in their care record. Flag charts that require interpreter services for every care interaction.
ADA Requirements for Home Care
The Americans with Disabilities Act requires home care agencies to provide reasonable accommodations for patients with disabilities. This includes providing documents in accessible formats (large print, Braille, audio), ensuring effective communication with patients who have hearing or vision impairments, and modifying care practices to accommodate physical or cognitive disabilities without reducing the quality of care.
ADA Compliance is Not Optional
Home care agencies that receive any federal funding (including Medicare or Medicaid) are subject to both the ADA and Section 504 of the Rehabilitation Act. Even private-pay-only agencies are covered by Title III of the ADA as places of public accommodation. Failure to provide reasonable accommodations can result in civil rights complaints, lawsuits, and loss of licensure.
Staff Training on Patient Rights
Training staff on the home care bill of rights is not a one-time event. It must be incorporated into new hire orientation and reinforced through annual training. Every employee who interacts with patients—from caregivers to office staff to schedulers—must understand their obligations.
Common Patient Rights Violations
These are the most frequently cited patient rights violations in state licensing surveys and CMS audits. Each violation can result in deficiency citations, corrective action requirements, and potential penalties.
Failing to provide written notice of rights before or at the start of services
CriticalIntegrate rights documentation into your intake checklist and home care software workflow.
No signed acknowledgment of receipt on file for active clients
HighUse electronic signature capture at intake. Audit charts quarterly for missing acknowledgments.
Discussing patient information in front of other clients or unauthorized persons
HighTrain caregivers on PHI confidentiality in shared living environments.
Retaliating against patients who file complaints or refuse services
CriticalEstablish anti-retaliation policy. Separate complaint handlers from care delivery staff.
Not informing patients of care plan changes before implementation
MediumRequire supervisor approval and patient notification before any care plan modification.
Fee changes without adequate advance written notice
MediumSend rate increase letters at least 30 days before effective date with new service agreement.
Frequently Asked Questions
Sources & References
Centers for Medicare & Medicaid Services
Conditions of Participation 42 CFR Part 484, patient rights requirements, and home health agency survey protocols.
Americans with Disabilities Act
ADA requirements for healthcare providers, reasonable accommodation guidance, and compliance resources.
HHS Office for Civil Rights
HIPAA enforcement, language access guidance under Title VI, and patient rights complaint investigation procedures.
State Departments of Health
State-specific home care licensing regulations, patient bill of rights requirements, and complaint hotline information.
Protect Patient Rights with Better Documentation
AveeCare's home care software includes built-in patient rights documentation workflows, HIPAA-compliant communication tools, and disclosure tracking to help your agency maintain compliance with all patient rights requirements effortlessly.
Sources & Disclaimer
Information in this guide is compiled from CMS Conditions of Participation, HIPAA regulations, ADA.gov guidance, HHS Office for Civil Rights publications, and various state Departments of Health licensing regulations.
This guide is provided for informational and educational purposes only. It does not constitute legal or compliance advice. Home care agencies should consult with qualified legal counsel and their state licensing agency for specific requirements.
Last updated: April 2026. AveeCare reviews and updates compliance information annually.