Home Care Interoperability: Health Data Exchange Standards & Implementation
Interoperability in home health care is no longer optional. CMS regulations, the 21st Century Cures Act, and the TEFCA framework are driving home care agencies to exchange health data electronically with hospitals, physicians, pharmacies, and payers. This guide explains the standards (FHIR, HL7, C-CDA), regulatory requirements, and practical steps for home care data integration -- including an interactive readiness assessment and implementation checklist. If you are planning an EHR rollout, our EHR implementation guide covers the migration process end-to-end.
Why Interoperability Matters for Home Care
Interoperability in home health is the ability to seamlessly exchange patient data between different healthcare systems. For home care agencies, poor health data exchange in home care leads to duplicated assessments, missed critical information from hospital discharges, delayed medication reconciliation, and billing errors. When home care data integration fails, patients are at risk and agencies lose revenue.
The stakes are rising. CMS now requires hospitals to send ADT (admission, discharge, transfer) notifications to post-acute providers including home health agencies. The 21st Century Cures Act prohibits information blocking. And TEFCA is creating a nationwide network for health data exchange that home care agencies will increasingly need to participate in. Agencies that invest in interoperability now will be positioned for better care coordination, fewer claim denials, and compliance with evolving regulations. For help evaluating EHR platforms with strong interoperability features, see our home care EHR selection guide.

CMS Interoperability Rules Affecting Home Health
Multiple federal regulations now mandate or incentivize health data exchange for home care agencies. Understanding these requirements is essential for compliance and for building an interoperability strategy that meets current and future mandates.
21st Century Cures Act
2016 / Rules 2020+- Prohibits information blocking by healthcare providers
- Requires support for patient access to their health data
- Mandates use of certified health IT with standard APIs
- Penalties for practices that restrict data access
CMS Interoperability Final Rule
2020 / Updated 2024- Requires FHIR-based Patient Access API for CMS-regulated payers
- Payer-to-payer data exchange requirements
- Provider directory API requirements
- Prior authorization API standards (Da Vinci)
ADT Notification Requirements
2021+- Hospitals must send electronic ADT notifications to post-acute providers
- Home health agencies should be able to receive and act on ADT data
- Supports timely care transitions and reduces readmissions
- Uses HL7 v2 ADT messages or FHIR-based alternatives
TEFCA
2024+- Trusted Exchange Framework and Common Agreement
- Creates nationwide health information exchange network
- QHINs serve as intermediaries for data exchange
- Single on-ramp to exchange with any participating entity
Health Data Exchange Standards Comparison
Understanding the major health data standards is crucial for planning your home care data integration strategy. Click on each standard below to explore its strengths, weaknesses, and use cases. FHIR is the standard most agencies should prioritize for new integrations, while HL7 v2 and C-CDA remain important for legacy connections.
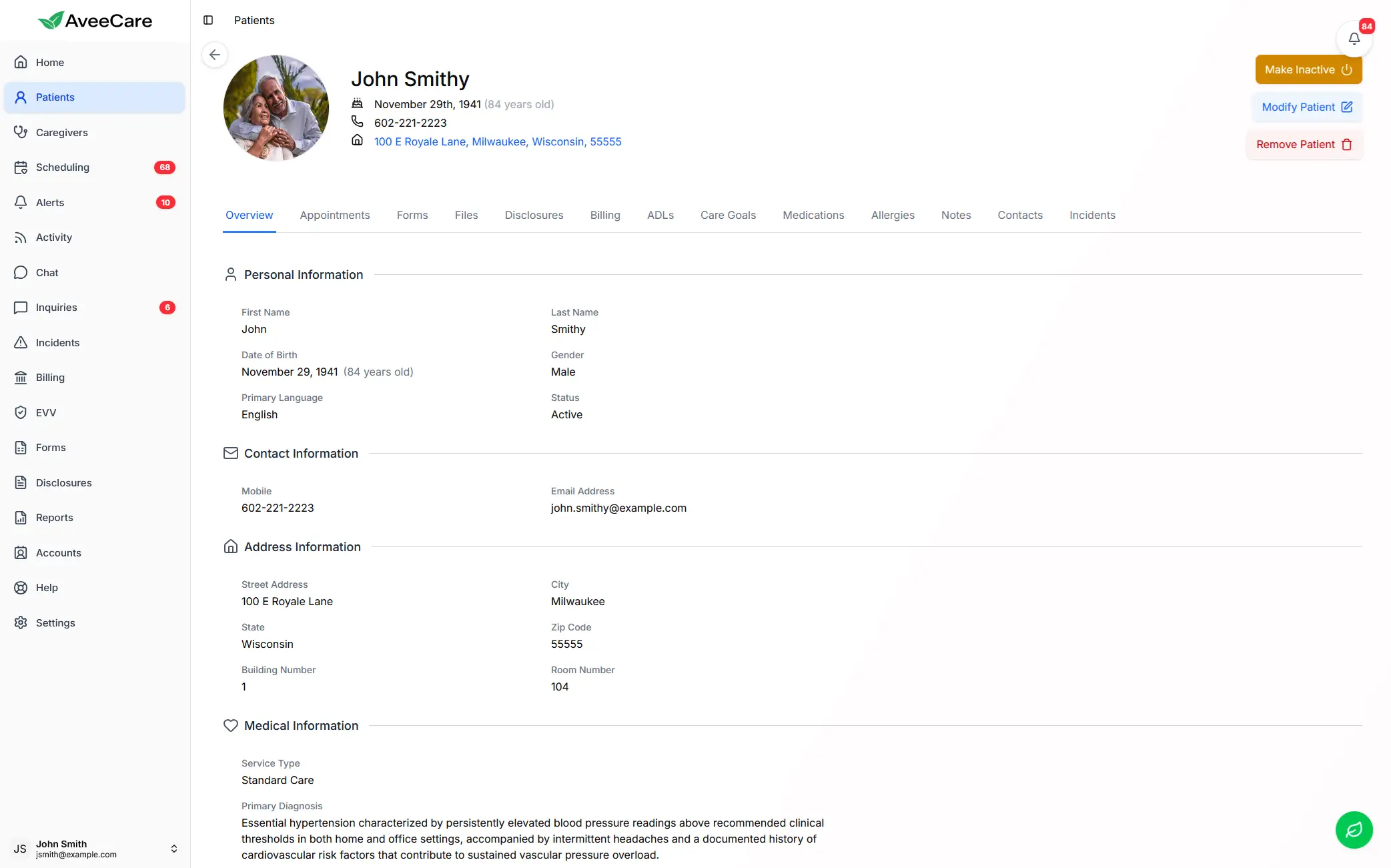
AveeCare patient overview showing integrated health data for coordinated home care
Interoperability Readiness Assessment
Rate your agency across six key areas to evaluate your current health data exchange capabilities and identify priority improvements.
Does your current home care software provide APIs for data exchange?
Is your agency connected to a Health Information Exchange?
Can your agency receive and act on hospital ADT notifications?
Does your agency have formal data governance policies?
Is your team prepared to work with electronic data exchange workflows?
Does your software vendor have a clear interoperability roadmap?
Common Integration Points for Home Care
Home care agencies need to exchange data with multiple partners. Each integration point has different requirements, standards, and benefits. Prioritize based on your referral sources, payer mix, and regulatory requirements.
Hospitals & Health Systems
Receive ADT notifications, discharge summaries, and referrals. Send patient updates and outcomes back.
HL7 v2 ADT, C-CDA, FHIRPhysician Offices
Exchange care plans, progress notes, medication lists, and orders. Coordinate ongoing care.
C-CDA, FHIR, Direct messagingPharmacies
Medication reconciliation, prescription verification, and drug interaction alerts.
NCPDP SCRIPT, FHIRLabs & Diagnostics
Receive lab results and diagnostic reports. Send orders for home-based testing.
HL7 v2 ORU, FHIRPayers & MCOs
Claims submission, eligibility verification, prior authorization, and remittance advice.
X12 EDI, FHIR (Da Vinci)HIEs & QHINs
Participate in regional and national health information exchange networks for broad data access.
FHIR, TEFCA protocolsIntegration Implementation Checklist
Track your progress implementing interoperability across assessment, planning, implementation, and ongoing operations.
Assessment
Planning
Implementation
Training
Validation
Ongoing
ROI of Interoperability for Home Care
Investing in home care data integration delivers measurable returns through reduced manual data entry, fewer billing errors, faster referral processing, and improved care coordination outcomes.
Frequently Asked Questions
Sources & References
Federal Resources
Standards Organizations
Modern, Connected Home Care with AveeCare
AveeCare is built on modern cloud architecture designed for seamless health data exchange. With integrated patient management, AI-powered analytics, and a platform built for interoperability, AveeCare helps home care agencies stay connected and compliant.
Transparent pricing. No mandatory demos. Trusted across all 50 states.
Disclaimer: This article is for informational purposes only and does not constitute legal or regulatory compliance advice. Interoperability requirements vary by state and payer. Always consult the latest CMS and ONC regulations and a qualified health IT consultant for compliance decisions. Published April 3, 2026.