Medicaid Waiver Programs for Home Care: HCBS Waivers Explained
Medicaid waiver programs are a critical funding source for medicaid home care services. This guide explains HCBS waiver types, state-by-state programs, eligibility, provider enrollment, and compliance requirements for home and community based services.

What Are Medicaid Waiver Programs?
Medicaid waiver programs allow states to provide long-term care services in home and community settings rather than requiring individuals to enter nursing facilities. The term "waiver" refers to the fact that these programs waive certain standard Medicaid requirements, giving states flexibility to design programs that serve specific populations, geographic areas, or service models.
Home and community based services (HCBS) delivered through waiver programs include personal care, homemaker assistance, respite care, adult day health, and many other services that help individuals remain in their homes. For home care agencies, becoming a medicaid waiver home care provider opens access to a large and growing population of individuals who need care services funded through Medicaid. Agencies serving veterans should also explore VA home care benefits, and our billing guide covers how Medicaid waiver reimbursement fits into a multi-payer strategy.
HCBS Spending Is Growing Rapidly
In 2024, Medicaid spending on HCBS waiver programs exceeded $130 billion, surpassing institutional care spending for the first time. This shift reflects both policy priorities and individual preferences for home-based care. For home care agencies, this means expanding opportunities for medicaid home care services.
Waiver Type Comparison
Compare the four main types of Medicaid waiver programs to understand which ones your agency or clients may be involved with.
1915(c) - HCBS Waiver
The most common Medicaid waiver for home care. Allows states to provide home and community-based services to individuals who would otherwise require institutional care in a nursing facility or ICF.
Key Features
- Most widely used HCBS authority (300+ active waivers)
- States can target specific populations and geographies
- Must demonstrate cost neutrality vs. institutional care
- States can cap enrollment (waitlists allowed)
- Renewable every 5 years (initial 3-year or 5-year approval)
Eligibility Requirements
- Individual must meet institutional level of care
- Services must be cost-neutral vs. nursing facility placement
- States must provide quality assurance
- Requires CMS approval of waiver application
| Feature | 1915(c) | 1915(i) | 1915(k) | 1115 |
|---|---|---|---|---|
| Institutional LOC required? | Yes | No | Yes | Varies |
| Waitlists allowed? | Yes | No | No | Varies |
| Statewide required? | No | Yes | Yes | Varies |
| Enhanced FMAP? | No | No | Yes (6%) | No |
| Self-direction option? | Optional | Optional | Required | Optional |
State HCBS Waiver Finder
Select a state to see its active HCBS waiver programs, covered services, waitlist status, and EVV model.
Select a state above to view its HCBS waiver programs.
HCBS Waiver Eligibility Assessment
Answer these screening questions to get a preliminary indication of whether an individual may qualify for medicaid waiver home care services.
What is the individual's age?
Is the individual's income below their state's Medicaid threshold?
How many ADLs does the individual need help with?
Does the individual have a cognitive impairment?
Where does the individual currently live?
Services Covered Under HCBS Waivers
The specific services covered under medicaid waiver programs vary by state and waiver type, but most HCBS waiver programs include the following service categories:
Personal Care
Assistance with bathing, dressing, grooming, toileting, and other ADLs
Homemaker Services
Light housekeeping, laundry, meal preparation, and grocery shopping
Respite Care
Temporary relief for unpaid family caregivers, in-home or facility-based
Adult Day Health
Structured programs providing social activities, meals, and health monitoring
Home-Delivered Meals
Nutritious meals delivered to homebound individuals
Transportation
Non-emergency medical and non-medical transportation
Home Modifications
Ramps, grab bars, widened doorways, and other accessibility improvements
Assistive Technology
Devices that help individuals perform daily tasks independently
Case Management
Care coordination, service planning, and ongoing monitoring
Provider Enrollment Process
Becoming an enrolled medicaid waiver home care provider requires meeting state-specific requirements. Here is the typical enrollment process:
Obtain state home care license
Meet all state licensing requirements for home care agencies, including administrator qualifications, office requirements, and staffing standards.
Meet insurance and bonding minimums
Maintain required general liability ($1M+), professional liability, workers compensation, and surety bond coverage at carrier-specified minimums.
Complete Medicaid provider application
Submit the state-specific Medicaid provider enrollment application with all supporting documentation. Many states now accept electronic applications.
Pass background checks and site survey
Complete ownership and controlling interest disclosures, pass criminal background checks, and host a state site survey or inspection.
Demonstrate EVV compliance
Show that your agency has a compliant EVV system in place that meets the state aggregator requirements for the 21st Century Cures Act.
Complete provider training
Complete any state-required provider orientation, billing training, and program-specific training modules.
Sign provider agreement
Execute the Medicaid provider agreement, which outlines your obligations, reimbursement rates, billing procedures, and compliance requirements.
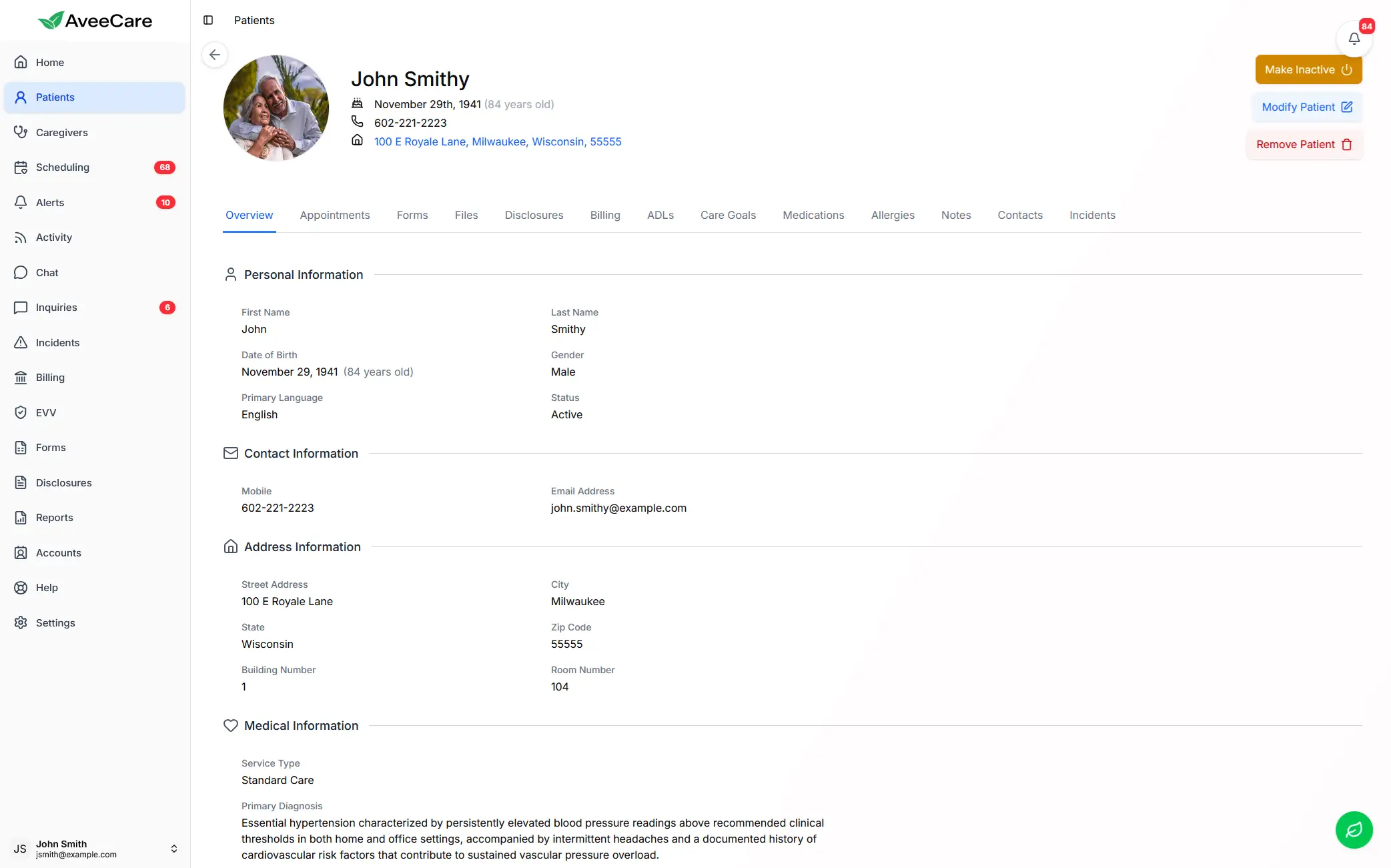
AveeCare's patient management helps agencies track eligibility, authorizations, and services for Medicaid waiver clients.
EVV Integration & Compliance Requirements
The 21st Century Cures Act mandates Electronic Visit Verification (EVV) for all Medicaid-funded personal care services. This is a critical compliance requirement for medicaid home care providers.
EVV Must Capture:
- Type of service performed
- Individual receiving the service
- Date of the service
- Location of service delivery
- Individual providing the service
- Time the service begins and ends
Other Compliance Requirements:
- Person-centered service planning
- Quality assurance and improvement
- Incident reporting and management
- Caregiver background checks
- Training and certification maintenance
- Financial and billing audits
Navigating Medicaid Waiver Waitlists
Over 800,000 people are currently on HCBS waiver waitlists across the country. Here are strategies agencies can share with families to navigate the wait:
Apply to multiple waiver programs
Individuals may qualify for more than one waiver. Apply to all applicable programs simultaneously, as waitlist times vary significantly.
Request priority or emergency placement
Many states have emergency or priority slots for individuals at immediate risk of institutionalization, homelessness, or abuse/neglect.
Explore 1915(i) and 1915(k) alternatives
These programs cannot have waitlists. If your state offers them, they may provide services while waiting for a 1915(c) waiver slot.
Contact your state Medicaid ombudsman
Long-term care ombudsmen can advocate for expedited placement and help families understand their options.
Consider bridge funding
Some states offer limited state-funded services for individuals on waiver waitlists. Private pay or LTCI can also bridge the gap.
Stay in contact with the state
Keep contact information updated, respond promptly to all requests, and check in quarterly on waitlist position.
Frequently Asked Questions
Sources & References
- CMS — Home & Community-Based Services Authorities
- Medicaid.gov — HCBS Waivers Section 1915(c)
- Kaiser Family Foundation — Medicaid HCBS Enrollment and Spending
- MACPAC — Medicaid and CHIP Payment and Access Commission
- CMS — 21st Century Cures Act EVV Requirements
- Administration for Community Living — HCBS Quality
Important Disclaimer: Medicaid waiver programs, eligibility criteria, covered services, and reimbursement rates vary significantly by state and change frequently. The state data in this guide is based on publicly available information as of early 2026 and may not reflect the most current program details. Always verify current program details directly with your state Medicaid agency. This guide is for informational purposes only and does not constitute legal, financial, or healthcare advice.
Manage Medicaid Waiver Services with Built-In EVV Compliance
AveeCare helps home care agencies manage client eligibility, track authorizations, document services, and maintain EVV compliance for Medicaid waiver programs.